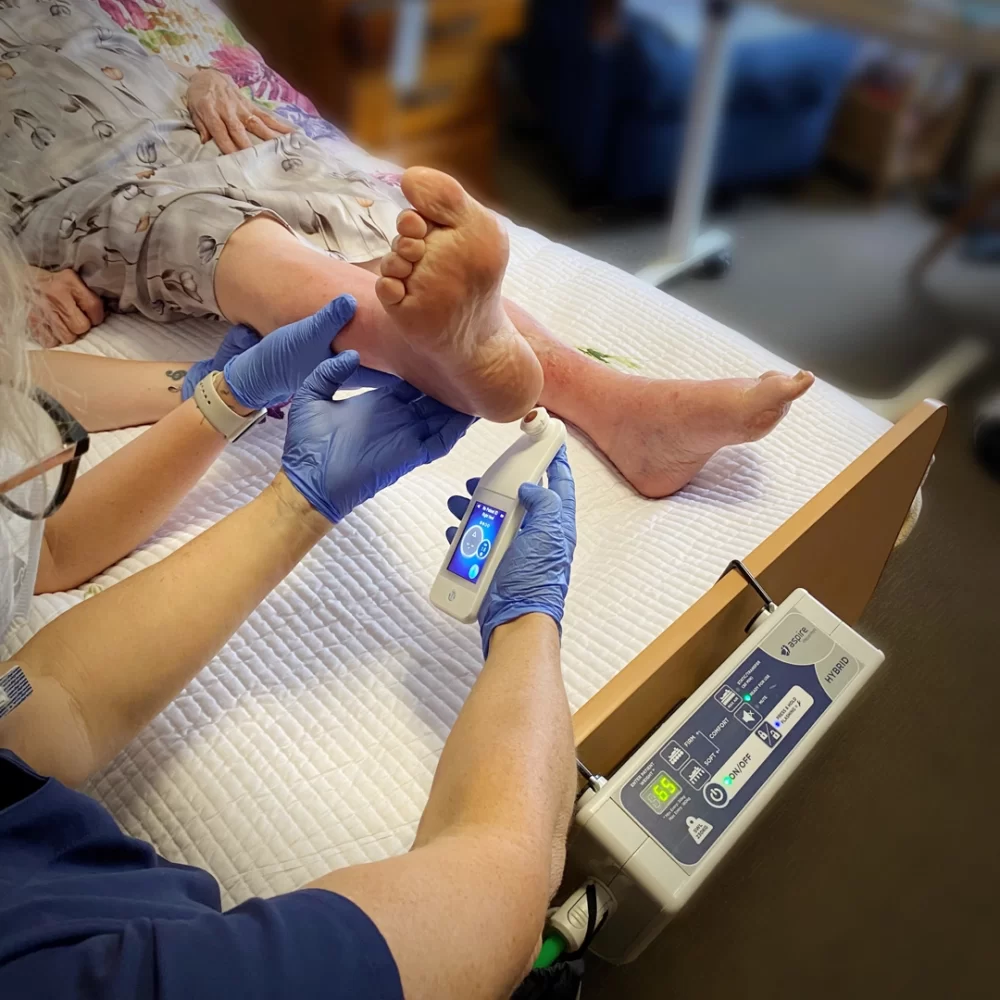
A first for Australian aged care providers, Peninsula Villages has introduced a new technology to its aged care facilities that can assist with the early detection of pressure injuries amongst residents. Created in the UK, the Provizio SEM Scanner supports clinicians to identify increased risk of pressure injuries up to five days earlier than visual skin assessments can, enabling them to take a preventative approach to treatment.
Pressure injuries, also known as pressure ulcers or bedsores, are defined as localised damage to the skin and/or underlying tissue, which usually occur over a bony prominence. These injuries typically arise from pressure, friction, and shear which leads to deformation within tissues and cells. Typically, the location of pressure injuries includes the heels or the sacrum area, with those who are older or have less mobility at a higher risk of developing them.
Central Coast aged care provider Peninsula Villages encompasses three residential aged care communities offering distinct levels of care including aged care, dementia care, palliative care and respite care to more than 300 residents. The innovative aged care provider has recently obtained this new device from market-leading supplier of medical devices and solutions, Arjo, and is excited to introduce it as part of its preventative care plan for residents.
“The Provizio SEM Scanner is a non-invasive hand-held device that assists in preventing pressure injuries,” explained Peninsula Villages’ Executive Care Manager, Steve Wills.
“By using this sub epidermal moisture scanning device, we will be able to detect changes under the skin that suggest the early onset of pressure damage that could later lead to ulcers. This is a particularly important early warning system because most pressure sores do not heal easily and require regular treatment or hospitalisation,” he continued.
It is estimated that the total cost of pressure injuries in Australian public hospitals in 2020 was $9.11 billion per year, of which treatment cost was $3.59 billion*. Furthermore, there were over 12,000 pressure injuries in all residential aged care facilities in the first three months of 2020, according to the National Aged Care Mandatory Quality Indicator Program.
Pressure injuries and pressure ulcers represent a significant clinical and financial burden for both aged care providers and hospitals worldwide,” continued Mr Wills.
“Pressure injuries can occur 3 to 10 days before becoming visible through inflammatory changes in the skin and underlying tissues. Injuries can develop quickly with irreversible damage occurring in vulnerable residents within a matter of hours.
“For us as a residential aged care provider, we aim to ensure we can properly prevent and treat our residents for any underlying or developing health issues that would normally lead to hospitalisation.
“Having this innovative new technology available, means our team of clinicians, nurses and carers can take on a preventative approach rather than a reactive one,” concluded Mr Wills.
The Provizio non-invasive technology is now being introduced to Registered Nurses and Assistants in Nursing across Peninsula Villages’ care facilities with the team excited by the new device and its abilities.
“This is a huge and innovative step for us in terms of how we provide our care and the approach we can take to assist with our residents’ overall wellbeing and care needs,” said Peninsula Villages’ CEO, Colin Osborne.
“Our team is hugely supportive of the device because it contributes to residents’ overall wellbeing and provides a further opportunity for residents to be involved in the delivery of their care through education and assessment,” he said.
sula Villages on the NSW Central Coast which accommodates 300 residents across its three residential care facilities. With more than 350 staff, Colin wants to highlight the mounting issues that face aged care workers and providers in the current climate.
“As an aged care provider, we of course welcome last week’s federal budget for its commitment to implement royal commission reforms, but do want to emphasise the remaining shortfalls in funding and workforce,” explained Mr Osborne.
“As an independent, not-for-profit aged care provider, we, like many others in the industry, are battling a workforce crisis and while we have managed to get creative with recruitment and development of staff, the real issue here is the huge droves of skilled staff who are leaving the industry for good.
“The reality is these people are feeling fed up and are leaving the sector due to the pay, conditions and quite frankly, brighter prospects in other fields,” he continued.
But the voices left out of this important conversation so central to this sector are the voices of the workers themselves.
“It was just last week that someone mentioned to me, you could be paid more in a retail or cleaning job than that of a caring and passionate aged care worker who is required to have an advanced set of skills. Quite simply, the existing award rates do not reflect the value and skills of the sector,” added Mr Osborne.
“With most residential aged care providers running at substantial losses, the government needs to step up and bridge the pay gap,” he explained.
It was in August this year that the Federal Government promised to pick up the bill for any potential pay rise for aged care workers in a submission to the Fair Work Commission (FWC). If the case is successful, the minimum wage of a qualified personal carer could increase from $23.09 to $28.86 an hour. A full-time level 1 aged care worker could see their weekly pay increase almost $200 a week.
“We are eagerly awaiting any outcome to increased pay for our sector, and while any rise is welcomed, there needs to be a national response as to how we will attract, retain and develop a skilled workforce in the future too. It’s a shame this wasn’t reflected in last week’s budget,” continued Mr Osborne.
In addition to pressures resulting from the COVID-19 pandemic, many providers fear that proposed reforms set out by the aged care royal commission cannot be realistically implemented, as the sector struggles with a lack of qualified aged care staff.
Whilst a pay increase for aged care staff may assist in promoting the attractiveness of employment in the sector it will not accelerate the availability of more people with the skills and qualifications required in aged care.
The skills shortage in aged care can only be addressed in the short term by attracting skilled staff back to the industry and potentially augmenting this with opportunities for skilled migration overseas. The longer-term solution, however, must be the development of more aged care specific training and qualification opportunities for Registered Nurses and care workers.
It is only with the availability of these additional people with appropriate skills that many of the recommendations from the royal commission into aged care can be genuinely and effectively implemented.
Whilst these challenges and constraints are reflected across the entire aged care sector, they represent factors which will place the very existence of aged care providers in rural and remote setting at risk.